Salam Sehat,
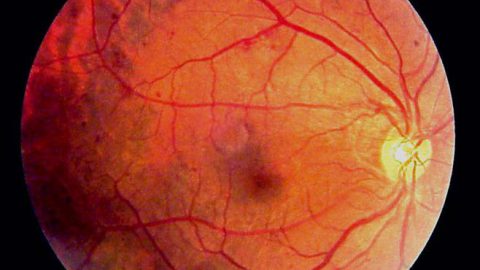
Retinopati diabetik adalah salah satu bentuk komplikasi diabetes melitus, di mana kadar gula yang tinggi pada akhirnya mengakibatkan kerusakan pada pembuluh darah retina mata, terutama di jaringan-jaringan yang sensitif terhadap cahaya. Kondisi ini dapat diderita oleh siapapun yang menderita diabetes tipe 1 maupun 2, terutama mereka yang gula darahnya tidak terkontrol dan telah menderita diabetes dalam jangka waktu yang lama.
Pada awalnya, retinopati diabetik seringkali hanya menunjukkan gejala ringan, atau bahkan tidak menimbulkan gejala sama sekali. Namun apabila tidak ditangani, retinopati diabetik dapat menyebabkan kebutaan. Maka dari itu, penderita diabetes melitus selalu disarankan untuk melakukan pemeriksaan mata rutin setidaknya satu kali dalam setahun meskipun tidak merasakan keluhan apapun pada mata.
Penyebab Retinopati Diabetik
Retina adalah sebuah lapisan di mata bagian belakang yang sensitif terhadap cahaya. Retina berfungsi mengubah cahaya yang masuk ke mata menjadi sinyal listrik yang akan diteruskan ke otak. Di otak, sinyal listrik ini akan diubah menjadi bentuk gambar yang kita lihat sehari-hari.
Karena fungsinya yang cukup penting tersebut, retina membutuhkan asupan darah yang lancar dari pembuluh-pembuluh darah kecil di sekitar retina. Pada penderita diabetes melitus, kadar gula darah yang terlalu banyak dapat menyumbat pembuluh-pembuluh darah kecil ini, sehingga retina pun kekurangan asupan darah.
Akibatnya, retina akan membentuk pembuluh darah baru guna mencukupi kebutuhan darah. Sayangnya, pembuluh-pembuluh darah yang baru terbentuk ini tidak mampu berkembang secara sempurna, sehingga rentan sekali pecah atau bocor.
Secara garis besar, retinopati diabetik dibagi menjadi dua jenis:
Retinopati diabetik non-proliferatif
Ini adalah stadium awal dari retinopati diabetik. Dikatakan non-proliferatif karena pada jenis ini, tidak terjadi pertumbuhan (proliferasi) pembuluh darah yang baru.
Retinopati diabetik non-proliferatif ditandai dengan adanya tonjolan kecil (mikroaneurisma) yang muncul dari pembuluh darah. Mikroaneurisma ini akhirnya akan menyumbat pembuluh darah vena, sehingga pembuluh darah vena menjadi mengembung dan berbentuk tidak rata. Apabila sumbatan semakin banyak dan luas, maka sistem persarafan dan makula (bagian inti dari retina) juga akan membengkak. Pembengkakan makula atau yang disebut juga makula edema ini merupakan kondisi yang membutuhkan penanganan segera.
Retinopati diabetik proliferatif
Retinopati diabetik proliferatif merupakan kondisi parah yang membutuhkan penanganan segera. Pada kasus ini, sebagian besar pembuluh darah retina telah rusak, sehingga terbentuklah pembuluh-pembuluh darah baru yang tidak normal. Pembuluh darah baru ini memiliki dinding yang lemah sehingga akan mudah pecah, dan darah akan merembes masuk ke cairan bola mata atau yang disebut dengan viterus. Bila semakin banyak, tumpukan cairan dan darah ini akan meningkatkan tekanan bola mata dan merusak persarafan, sehingga menyebabkan suatu kondisi yang disebut dengan glaukoma.
Selain itu, pertumbuhan pembuluh-pembuluh darah baru ini akan memicu terbentuknya jaringan parut. Jaringan parut ini pada akhirnya akan menarik retina sehingga terlepas bagian belakang mata. Pada saat ini terjadi, seseorang bisa mengalami gangguan pengelihatan.
Retinopati diabetik sangat mungkin dialami oleh penderita diabetes yang telah lama memiliki penyakit tersebut. Semakin lama seseorang memiliki diabetes maka semakin besar pula risiko untuk terkena retinopati diabetik, terutama apabila kadar gulanya tidak terkontrol. Selain itu, risiko juga akan meningkat jika didukung oleh faktor-faktor berikut ini:
- Kehamilan
- Memiliki kadar kolesterol dan tekanan darah yang tinggi
- Kebiasaan menghisap tembakau
- Beretnis Hispanik, berkulit hitam, atau merupakan penduduk asli Amerika.
- Menderita sindrom Down
Gejala Retinopati Diabetik
Awalnya, retinopati diabetik mungkin tidak menunjukkan gejala. Namun seiring kondisi berkembang, gejala-gejala dapat muncul dan biasanya memengaruhi kedua mata. Beberapa gejalanya adalah:
- Penglihatan menurun secara perlahan-lahan.
- Pengelihatan hilang mendadak.
- Tampak ada benda atau bercak hitam yang melayang-layang di lapangan pandang.
- Pengelihatan berbayang.
- Pengelihatan warna terganggu.
- Nyeri pada mata atau mata merah
Gejala-gejala tersebut tidak selalu berarti Anda mengalami retinopati diabetik, namun tidak ada salahnya untuk segera memeriksakan diri ke dokter. Lakukan juga pemeriksaan mata rutin walau Anda merasa tidak ada yang salah dengan kondisi mata agar penyakit dapat terdeteksi dan ditangani lebih awal.
Diagnosis Retinopati Diabetik
Untuk menegakkan diagnosis retinopati diabetik, dokter perlu melihat kondisi di dalam bola mata Anda dengan suatu pemeriksaan yang disebut funduskopi. Kondisi di dalam bola mata seseorang akan paling jelas terlihat dalam keadaan pupil terbuka lebar. Maka dari itu, dokter mungkin akan memberikan obat tetes mata yang bertujuan untuk melebarkan pupil Anda. Obat tetes mata tersebut dapat membuat pengelihatan jangka pendek Anda menjadi kabur, namun hal ini hanya akan berangsur-angsur menghilang saat efek obat sudah habis.
Pada saat melakukan funduskopi, dokter akan mencari beberapa hal berikut:
- Pembuluh darah yang tidak normal
- Pembengkakan serta tumpukan darah dan lemak di retina
- Pertumbuhan pembuluh darah baru dan jaringan parut
- Perdarahan di cairan bola mata (vitreus)
- Terlepasnya lapisan retina
- Kelainan di saraf mata
Untuk melihat ada tidaknya kelainan di pembuluh darah mata, terutama pembuluh darah yang baru terbentuk, dokter biasanya akan melakukan suatu pemeriksaan yang disebut dengan angiografi fluoresensi. Pada pemeriksaan ini, Anda akan diberikan obat tetes untuk melebarkan pupil, kemudian dokter akan menyuntikkan sebuah pewarna khusus di lengan Anda. Cairan pewarna ini pada akhirnya akan mengisi pembuluh darah di bola mata Anda, dan dokter akan mengambil gambar keadaan pembuluh darah di dalam bola mata dengan menggunakan alat khusus. Dari situ akan tampak jelas ada tidaknya penyempitan atau pecahnya pembuluh darah, serta ada tidaknya kebocoran cairan.
Prosedur lain yang mungkin dilakukan adalah melakukan pemeriksaan optical coherence tomography (OCT) yang akan memberikan gambaran ketebalan retina mata. Dari pemeriksaan ini, akan tampak secara jelas jika terjadi kebocoran cairan ke dalam jaringan retina. Pemeriksaan OCT juga dapat digunakan untuk menentukan keberhasilan terapi.
Pengobatan Retinopati Diabetik

Pilihan pengobatan retinopati diabetik bergantung dari jenis dan derajat keparahan penyakit, yakni:
- Retinopati diabetik non-proliferatif. Pada tahap ini, penderita mungkin belum memerlukan perawatan melainkan akan dimonitor terlebih dahulu oleh dokter. Penderita akan dianjurkan untuk kontrol rutin ke dokter mata dan dokter ahli diabetes (endokrinologi), serta belajar mengendalikan kadar gula dalam darah karena langkah ini biasanya dapat memperlambat perkembangan penyakit.
- Retinopati diabetik proliferatif. Pada tahap ini terdapat beberapa prosedur operasi yang mungkin direkomendasikan kepada penderita, antara lain:
Suntikan anti-VEGF ke dalam mata – Suntikan ini diberikan langsung ke dalam mata dan berguna untuk mencegah pembentukan pembuluh darah baru di bagian belakang mata. Suntikan diberikan sebanyak satu kali sebulan, dan perlahan-lahan dikurangi atau dihentikan saat kondisi telah stabil. Beberapa efek samping yang mungkin muncul, adalah iritasi mata, merasa ada sesuatu di dalam mata, mata berair atau gatal, perdarahan, hingga pembekuan darah.
Vitrektomi – Operasi ini bertujuan untuk mengeluarkan darah dan jaringan parut dari bagian tengah mata dengan cara membuat irisan kecil pada mata dengan bantuan anestesi umum maupun lokal.
Perawatan dengan sinar laser fokal atau fotokoagulasi – Perawatan dengan sinar laser ini bertujuan untuk memperlambat atau menghentikan titik-titik kebocoran cairan atau darah di dalam mata.


Perawatan dengan sinar laser yang menyebar atau fotokoagulasi panretinal – Sedikit berbeda dengan sinar laser fokal, pada perawatan ini fokus sinar yang diberikan lebih luas, sehingga dapat mengenai suatu area tertentu di bagian retina secara langsung. Terapi sinar laser ini akan membakar pembuluh-pembuluh darah baru yang tidak normal sehingga menyusut dan akhirnya menjadi jaringan parut.
Selain obat pereda rasa sakit, dokter akan menyarankan pasien untuk tidak mengoperasikan kendaraan atau mesin berat serta menggunakan kacamata hitam.
Komplikasi Retinopati Diabetik
Jika tidak segera diobati, pembuluh darah baru yang tumbuh secara tidak normal di retina dapat menyebabkan gangguan penglihatan yang serius hingga kebutaan. Beberapa komplikasi retinopati diabetik yang mungkin terjadi, antara lain:
- Perdarahan vitreus – Pembuluh-pembuluh darah yang baru terbentuk akan rentan pecah, sehingga darah akan masuk ke bagian tengah mata. Jika darah yang bocor hanya sedikit, Anda mungkin hanya akan melihat bayangan gelap yang melayang-layang di lapangan pandang Anda. Semakin banyak darah yang bocor maka semakin terhalang pula penglihatan. Walau darah dapat berangsur-angsur menghilang dalam hitungan minggu atau bulan, penderita tetap berisiko kehilangan penglihatannya secara permanen jika retina telah rusak.
- Terlepasnya retina – Pembuluh darah baru yang muncul akibat retinopati diabetik akan merangsang pembentukan suatu jaringan parut di lapisan retina. Jaringan parut inilah yang kelak berisiko untuk menarik retina lepas dari dasarnya, sehingga dapat memunculkan gejala-gejala seperti pengelihatan kabur, muncul gambaran tirai di lapangan pengelihatan, tampak kilatan cahaya, atau bahkan kebutaan.
- Glaukoma – Ketika pembuluh darah tumbuh di bagian depan mata, saluran air mata dapat tersumbat, sehingga cairan akan menumpuk di bola mata dan tekanan bola mata akan meningkat. Kondisi peningkatan tekanan di dalam bola mata ini disebut dengan glaukoma. Glaukoma dapat merusak saraf-saraf pengelihatan, sehingga dapat menyebabkan gangguan pengelihatan.
- Kebutaan – Pada akhirnya retinopati diabetik, glaukoma, atau keduanya dapat menyebabkan kebutaan.
Pencegahan Retinopati Diabetik
Mengatur kadar gula darah dengan baik adalah salah satu cara menghindari hilangnya penglihatan. Berikut adalah langkah-langkah lain yang bisa dilakukan:
- Lakukan kegiatan aerobik, seperti jalan kaki setidaknya selama dua setengah jam setiap minggu.
- Memulai diet makan yang sehat dan berimbang yang sesuai dengan kondisi Anda. Kurangi juga asupan gula, garam, dan lemak.
- Mengurangi berat badan, bagi pemilik kondisi obesitas.
- Berhenti mengonsumsi minuman beralkohol.
- Berhenti merokok atau menghisap tembakau.
- Minum obat diabetes atau insulin sesuai anjuran dokter
- Pantau kadar kolesterol Anda.
- Pantau kadar gula darah Anda melalui tes gula darah sesuai dengan instruksi dokter.
- Diskusikan bersama dokter mengenai tes hemoglobin A1C yang mungkin bisa Anda lakukan selain tes gula darah.
- Selalu waspada jika merasakan perubahan pada penglihatan Anda.
Pemeriksaan mata dan tekanan darah yang rutin juga merupakan langkah pencegahan awal agar penyakit tidak berkembang menjadi lebih buruk.
Sumber : alodokter.com
Ilustrasi :
- Dok. RS Kasih Ibu
- emedicine.medscape.com
- wadeopticians.com

